Should obese women be denied fertility treatments on parental and child health grounds? Fertility conference.

 Or should we look at the causes of fatty liver?
Or should we look at the causes of fatty liver?

 Or should we look at the causes of fatty liver?
Or should we look at the causes of fatty liver?
 Medical professionals have recently published guides to reducing insulin and other diabetes medications for patients on low carbohydrate diets because many of these patients are suddenly getting better. Their improvement and sometimes remission carries a diminishing need for insulin or oral antihyperglycaemics. If doctors and nurses fail to realise this, their patients risk overdose, with potentially rapidly fatal results - and not just with where insulin is concerned. This means that a new approach to diet for both main types[1] of diabetic - Types 1 and 2 - is making a big difference. In some cases it is effecting complete remission.
Medical professionals have recently published guides to reducing insulin and other diabetes medications for patients on low carbohydrate diets because many of these patients are suddenly getting better. Their improvement and sometimes remission carries a diminishing need for insulin or oral antihyperglycaemics. If doctors and nurses fail to realise this, their patients risk overdose, with potentially rapidly fatal results - and not just with where insulin is concerned. This means that a new approach to diet for both main types[1] of diabetic - Types 1 and 2 - is making a big difference. In some cases it is effecting complete remission.
Diabetes is big business and so it should not surprise us to hear that there are commercial forums to attract and market to diabetes sufferers. There are also free forums, like https://healthunlocked.com/, which I prefer. However, the other day I found an article in diabetes.co.uk, entitled, "Healthcare professionals publish low carb diabetes medication guide." I was interested in this because it clearly shows the beneficial impact of low carb high fat diets on diabetes 2, a modern day epidemic. What has happened is that people are curing themselves of diabetes 2 or substantially improving it, by changing from starchy diets to high fat low carbohydrate diets. Further reading also indicated improvement in Diabetes 1. [2] These improvements are obviously so important that doctors are being forced to lower or stop anti-hyperglycaemic medications, including insulin and oral drugs, because these (especially insulin) can cause rapid coma and death in patients who no longer need them, or who suddenly require lesser doses. High blood pressure also frequently reduces, making anti-hypertensives potentially dangerous.
There are two types of life-threatening coma involved in diabetes. One comes with the disease and the other is iatrogenic - or doctor/medically caused. Few patients or professionals ever think this through.[3] The first kind is from high glucose and the second is from low glucose. The first and original diabetes coma comes with the patient's inability to produce insulin to process food that breaks down to glucose, hence glucose builds up to abnormal levels in the blood and causes dysfunction and death eventually. This kind of coma usually builds slowly, over days. The second kind, or medically-caused, comes from treatment with insulin, which is prescribed for patients who cannot produce enough insulin to process glucose. Insulin comas can occur within minutes and hours, ending quickly in death when unattended and risking brain injury when attended. Before insulin treatment, insulin comas did not occur in diabetes. Insulin comas may also occur in Type 2 diabetics treated with oral antihyperglycaemics. (See, for instance, Gian PaoloFadini et al, Characteristics and mortality of type 2 diabetic patients hospitalized for severe iatrogenic hypoglycemia, Diabetes Research and Clinical Practice Volume 84, Issue 3, June 2009, Pages 267-272.) To my mind, this places a very sombre perspective on Type 2 diabetes, treated with traditional low fat diets and oral antihyperglycaemics. Patients should therefore be made aware, as a matter of urgency, of the success of high fat low carbohydrate diets in removing or reducing the need for oral antihyperglycaemics or injectable insulins.
There is an obvious association between agricultural civilisations and diabetes. Diabetes was probably extremely rare among hunter gatherers, and it is thought that Australian Aborigines did not suffer from the disease until they were exposed to flour, sugars and alcohol, with European take-over of Australia. In hunter-gatherer societies, healthy humans create glucose from animal protein, but they may also access it from modest amounts of vegetables and fruits in season. In contrast, agricultural societies have introduced to human diets unnaturally large quantities of carbohydrate, via sugary and starchy vegetables, grains and fruits. Wheat, corn, fruit, potato, and their products - flour, rice, corn, bread, cake, candy, pasta, fries, chips, tacos, corn-syrup/fructose, and abnormally abundant fruit in and out of season. Among the first reports of diabetes came from the agricultural society of Ancient Egypt, where doctors tasted patients' urine (which is normally fairly sterile due to our complex filtration systems) and diagnosed diabetes when it was sweet. In India doctors noticed that ants were attracted to high glucose urine.
For a century or so, as diabetes has become more and more a feature of 'modern' life, doctors and dieticians have been performing dietary gymnastics in order to somehow keep diabetics eating the modern diet. A belief has come about that humans require starches and fruits, in order to survive and make glucose. Whilst non-starchy vegetables and fruits contain helpful nutrients and are not too difficult to break down for most people, starches and fruits are dangerous for diabetics and, as I pointed out above, appear to exacerbate diabetes 1 and to cause diabetes 2. Diabetics have to take oral anti-hyperglycaemics or inject themselves with insulin in order to prevent the accumulation of glucose in their blood when they eat these starches and fruits. So, why would dieticians continuously advocate these starches and fruits when drugs are required to generate insulin in order to avoid high glucose comas? Why would they advocate these when there is a high incidence of neurological complications and death from these drugs?
The reason appears to be received wisdom that humans not only need vegetables and fruit, but that they need wheat, bread, pasta, jam, tapioca, corn, rice, fries, chips and several pieces of fruit daily, in and out of season. This is what the 'Food Pyramid' you still see in doctors' surgeries is all about.[4] This received wisdom fails to account for the success of hunter-gatherer diets and their very limited supplies of starches. A reason for this failure to reference these diets could be the belief that hunter-gatherers all died at around 30 years old - something that you will read in many places - even though it is patently untrue. You cannot rely on the average health professional to personally test the information they receive from 'respected authorities'. Influenced by 'modern' schooling and universities, they have been taught by people who actually believe that agricultural diets, because they accompanied modern civilisation - generally valued for its abundant technology and material wealth - must be better than pre-agricultural diets. Somehow the concomitant epidemic of diabetes causes too much cognitive dissonance to investigate, so it is just avoided.
Athough Allan Mazur writes that the "primacy of diet diminish[ed] once insulin became available [discovered 1922], leading to the primacy of medication. Weight loss apart, there is still today no evidence-based consensus on proper diabetic diets," he also notes the success of high fat low carbohydrate diets before insulin:
"Newburgh and Marsh report on 73 cases, apparently mostly adults, admitted to the University of Michigan Hospital, where the state's physicians referred their severest cases as a "court of last appeal." On entering the clinic, patients were not fasted but placed on a diet of 900-1,000 calories, high in fat, low in carbohydrate. After being sugar free for one or two weeks, the diet was increased from 1,400 to 2,500 calories, depending on the needs of the person, most calories coming from fat, least from carbohydrate. Excepting three patients who died within a day of admission, and another who "went into coma after eating a bag of oranges brought by a relative," the urine of all patients became sugar free, none developed severe acidosis, and the investigators were "greatly impressed by the excellent condition of our patients months after leaving the clinic".
I am not submitting the Michigan study as definitive, but it fortified the position of anti-starvation physicians who argued that carbohydrates were the main source of glucose in urine and blood, so it was unnecessary to starve patients as long as carbohydrate was limited, and for seriously ill children there was little that could be done in any case. Critics also claimed, as had Allen himself in 1913, that "fat feeding is not to be feared in diabetics." (Allan Mazur, Why were "starvation diets" promoted for diabetes in the pre-insulin period? Nutr J. 2011; 10: 23.) [5]
Probably the impetus to examine our modern diets and dietary needs logically has come from people who became afflicted with diabetes 2. With the rise of the internet, it has become much easier for these people to communicate with each other. Health professionals and scientists have been among their number, and the fact that doctors are now warning each other to reduce diabetic medication dosages because many people are recovering through low carb and high fat diets is significant.
[1] Diabetes insipidus is a different kettle of fish from diabetes 1 and 2.
[2] Diabetes 1 is probably not diet-caused, but it can be partly diet-treated and some people who have been diagnosed with diabetes 1 may experience remission with low-carb diets, arguably indicating that diet was involved in their diabetes, rather than pure lack of insulin production. Belinda S. Lennerz, et al, Management of Type 1 Diabetes With a Very Low–Carbohydrate Diet, Pediatrics June 2018, VOLUME 141 / ISSUE 6.
[3] In non-diabetics there are few major causes of hypoglycemia but it may occur in alcoholic crises, "critical illness, counter-regulatory hormone deficiencies, and non-islet cell tumors." People have also been known to receive or take insulin surrupticiously to induce coma or death. See, for instance, Philip Mathew; Deepu Thoppil: Hypoglycemia. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. https://www.ncbi.nlm.nih.gov/books/NBK534841/
[4] M Nestle, Food lobbies, the food pyramid, and U.S. nutrition policy. Int J Health Serv. 1993;23(3):483-96.https://www.ncbi.nlm.nih.gov/pubmed/8375951
[5] Allan Mazur, Why were "starvation diets" promoted for diabetes in the pre-insulin period? Nutr J. 2011; 10: 23.
Published online 2011 Mar 11. doi: 10.1186/1475-2891-10-23 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3062586/#B27
[5]

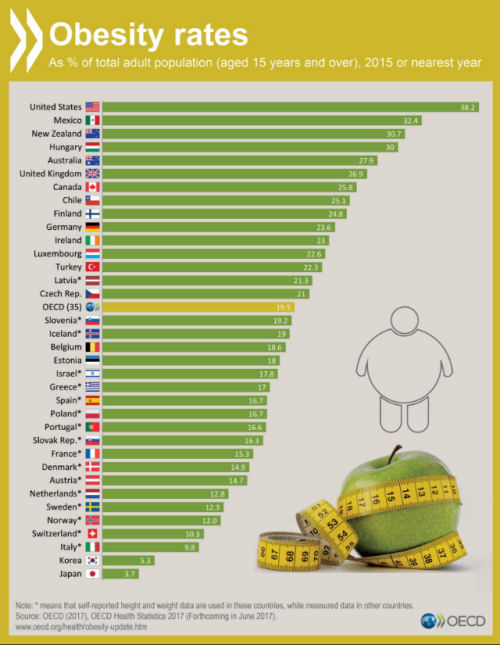
 The article by Robert Bridge, quoted and linked to inside, speculates on obesity being a factor in the United States' poor performance in the PyeongChang olympic games. It includes a graph of order of obesity in OECD countries. Australia is the fifth highest obesity country. Japan is the lowest. My money is on high fructose additions to our diets, such as corn-syrup. Dr Lustig University of California San Francisco, Division of Pediatric Endocrinology, has been putting this message out for some time in fascinating scientific videos, including, "Fat Chance" and "The skinny on obesity." I have embedded "Fat chance" in the quoted material from the article inside.
The article by Robert Bridge, quoted and linked to inside, speculates on obesity being a factor in the United States' poor performance in the PyeongChang olympic games. It includes a graph of order of obesity in OECD countries. Australia is the fifth highest obesity country. Japan is the lowest. My money is on high fructose additions to our diets, such as corn-syrup. Dr Lustig University of California San Francisco, Division of Pediatric Endocrinology, has been putting this message out for some time in fascinating scientific videos, including, "Fat Chance" and "The skinny on obesity." I have embedded "Fat chance" in the quoted material from the article inside.
Now that the Olympic torch in PyeongChang has been extinguished and the athletes and fans have gone home, the US is wrestling with its worst performance in 20 years. Could obesity rates be taking a toll on US athletic performance? On the surface, Team USA’s total haul of 23 medals, which included nine golds, seems rather respectable. It put the United States in fourth place, behind Norway, Germany and Canada. But not everyone went home satisfied, and least of all the US Olympic Committee, which had predicted US athletes would win at least 37 medals. Not only were the Americans bested by three countries which, combined, make up just one-third of the US population (Norway, which won 39 gold medals in PyeongChang, has just 5.2 million people), it was their worst performance since the 1998 Nagano Games. The situation looks even more troubling when we consider that the US fielded 242 athletes at PyeongChang, the largest-ever delegation in the history of the Winter Games.
The US has been spending wads of cash in an effort to get the most from its athletes. The amount forked over to Winter sports in the years 2015-16 increased by nearly six percent from the previous Olympic 2011-2012 cycle, AP reported. Alas, all that extra cash has produced little in way of gold. Since the 2010 Vancouver Games, America’s total medal haul in the Winter Games has been on the decline (37, 28 and 23, respectively).
“We have this amazing depth. We have these incredible medalists,” Alan Ashley, US chief of sport performance told reporters following the closing ceremony. He then ventured the question: “How do we continue to compete even at a higher level and give them what they need going forward?”
What is the source of this decline? Since it does not seem related to a lack of funding, or a shortage of potential athletes, could there be particular sociocultural reasons at play, for example particular health factors? As was already acknowledged by the US government back in 2012, when it partnered with Olympic and Paralympic athletes to get more than 1.7 million children involved in sports through Michelle Obama’s "Let's Move!" initiative, obesity is a serious issue that is only getting worse.
A recent study put out by the OECD predicts that by the year 2030, almost 50 percent of Americans will be considered as clinically obese. In 13 states, that number could actually exceed 60 percent.
While there seems to be little research to date on the subject, a 2016 policy paper put out by the American Development Model (ADM) in cooperation with the US Olympics Committee (USOC) suggests that America’s sporting officials are aware of the problem when it warned: “The percentage of obese children ages 6-11 increased from 7 percent in 1980 to 18 percent in 2010. Among children ages 12 to 19, that figure grew from 5 percent to 18 percent.” The paper goes on to detail how parents, schools and sporting clubs can alter their lifestyles and dietary choices to become better athletes.
Read more at https://www.rt.com/op-ed/420669-obesity-usa-olympics-pyeongchang/
Recent comments